Understanding the gaps: Why HPV vaccine uptake in Kenya remains worryingly low

During The Eastleigh Voice's visit to several informal settlements, many mothers believed their children had already been vaccinated against HPV, with some assuming it was included in the routine immunisation schedule
Franciscah Kanini, a community health volunteer (CHV) from Kitui village in Pumwani Majengo, carries the emotional and physical scars of cervical cancer.
Having experienced the devastating impact of the disease firsthand, she often reflects on how different her life might have been if the HPV vaccine had been available and if she had known about it earlier.
More To Read
- Kenya reports progress in HPV vaccination, still short of WHO target
- 10 runners race up Mt Kenya in 10 hours to honour women lost to cervical cancer
- Kamukunji rallies against vaccine myths as leaders take immunisation door-to-door
- African nations pledge to boost local manufacturing of medical products
- Kamukunji’s Kinyago Kanuku hosts groundbreaking breast and cervical cancer screening
- HPV blood test shows promise for early detection of multiple cancers, study finds
Today, Kanini is on a mission to prevent others from suffering the same fate. She visits homes across her community to raise awareness about the vaccine that protects against cervical cancer. However, her efforts face major obstacles, including misinformation, cultural myths and a general lack of awareness.
“In informal settlements like ours, many parents still don’t fully understand what the HPV vaccine is for," Kanini told The Eastleigh Voice. "The way information is shared often doesn’t match how people here learn best. It’s not simplified, it’s not in our language, and sometimes it’s not even trusted.”
One of the most common misconceptions Kanini encounters is the belief that the HPV vaccine is a form of early family planning.
“That’s one of the biggest barriers we face. Some parents believe the vaccine is meant to stop their daughters from having children in the future. Because of this misunderstanding, they’re hesitant to allow them to receive it,” said Kanini.
To counter this, Kanini and other CHVs hold community meetings, have one-on-one conversations, and even use church announcements to explain that the vaccine prevents cervical cancer. "We know the cost of not getting it, and we’re trying to prevent others from going through that pain," she said.
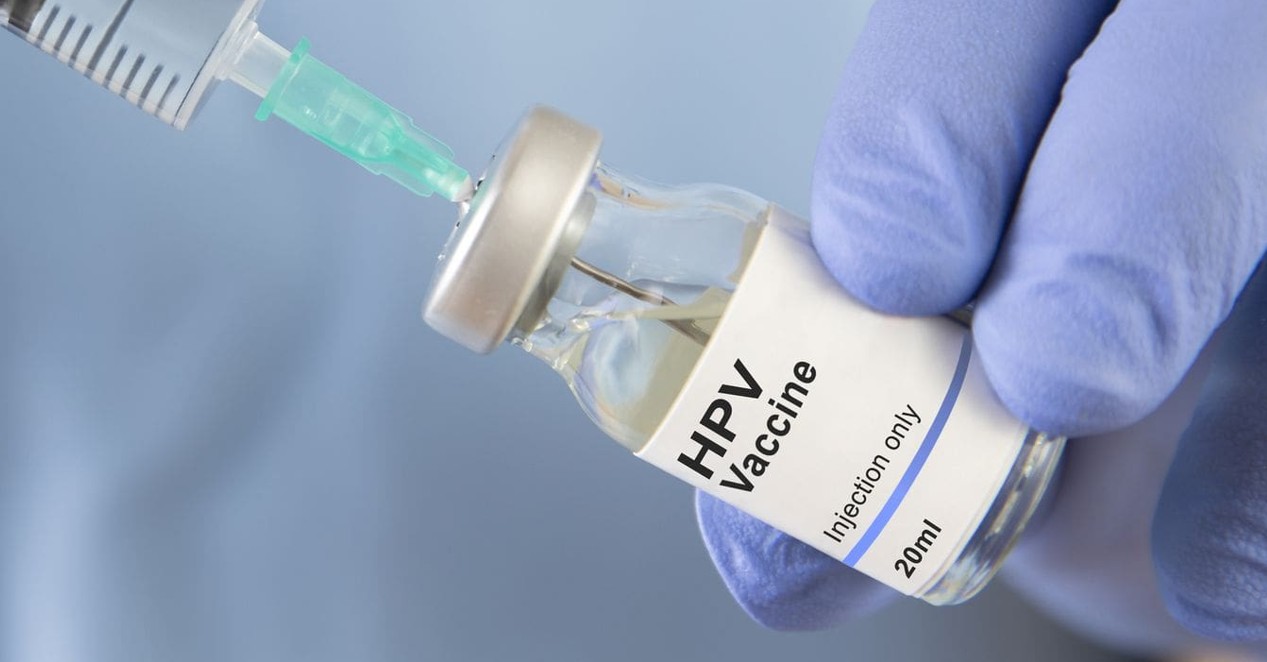 Single-dose HPV vaccine. (Photo: WHO)
Single-dose HPV vaccine. (Photo: WHO)
Despite these efforts, Kanini admitted the workload is overwhelming, “We’re dealing with large numbers of people and a heavy workload. There are simply not enough of us to reach everyone consistently. Sometimes we cover whole neighbourhoods alone, and it's exhausting. Even when people want to learn more, we don’t always have the time or resources to follow up properly.”
One recurring concern she often hears is why the vaccine is given only to girls when other vaccines are administered to both boys and girls.
"When we administered the typhoid vaccine, both boys and girls received it. But the HPV vaccine is different. It’s targeted at girls aged 9 to 14 because it’s meant to protect against cervical cancer, something that only affects women. Boys don’t have a cervix,” explained Kanini.
Adding, “It’s easier to prevent the infection than to treat the cancer years later. We need more community-friendly, clear, and culturally sensitive education around the HPV vaccine. When people understand the ‘why,’ they’re more willing to say yes.”
Kanini’s experience reflects a wider issue in Nairobi’s informal settlements, where many residents lack accurate information about the HPV vaccine.
During The Eastleigh Voice's visit to several informal settlements, many mothers believed their children had already been vaccinated against HPV, with some assuming it was included in the routine immunisation schedule, while others mistakenly thought that boys had also received the vaccine.
 Fatuma Wairimu. (Photo: Justine Ondieki)
Fatuma Wairimu. (Photo: Justine Ondieki)
Fatuma Wairimu, a mother of four from Kitui village in Majengo, is confident that her children, including her three sons, have received the HPV vaccine through routine immunisation campaigns.
However, Fatuma mistakenly thinks the vaccine protects against a range of diseases beyond HPV. In Kenya, the HPV vaccine is currently offered only to girls - unlike in some other countries where boys are also included in the program.
“The HPV vaccine protects children from HIV, TB, and many other diseases. It strengthens their bodies and helps them fight illnesses,” said Fatuma.
Similarly, Latifa Kioko, mother of a 12-year-old daughter, remains unsure about the vaccine’s purpose despite its rollout starting in 2019.
 Latifa Kioko. (Photo: Justine Ondieki)
Latifa Kioko. (Photo: Justine Ondieki)
“We have many questions,” Latifa told The Eastleigh Voice. “No parent wants to leave their child unprotected, but we need clear information. If campaigns explained it better, more women would come forward.”
Latifa noted that many parents who decline the vaccine do so not out of opposition, but due to a lack of clear and accessible information.
“Explain to us during the campaign, and women will come out. We need to understand how it helps. When information is broken down, in simple language we can understand, using examples that relate to our lives, it reaches us, and we take action,” said Latifa.
Michael Mwangi, a father of a 19-year-old daughter, had never heard of the HPV vaccine.
 Michael Mwangi (left). (Photo: Justine Ondieki)
Michael Mwangi (left). (Photo: Justine Ondieki)
Although the vaccine was introduced when his daughter was within the eligible age range, Mwangi admitted he missed the vaccination opportunity due to a lack of information.
He is now determined to ensure his granddaughter receives the vaccine, “If people understand how dangerous something is and how the vaccine can help, it would guide their decisions. Had I known about it and had clear information, I would have pushed for my daughter to be vaccinated. When people educate one another, it becomes easier."
Top Stories Today